Hip Resurfacing via the “No-Table” Direct Anterior Approach With Capsule Preservation: A Step-by-Step Guide
Introduction
"No-table" direct anterior total hip arthroplasty is becoming widely adopted around the world because it results in fewer injuries, allowing for faster recovery and, in some centers, same day surgery. Hip resurfacing arthroplasty is a more conservative form of hip arthroplasty with regard to bone preparation; however, it usually is performed via the posterior approach. Although these two techniques have been combined before, this video presents a step-by-step guide for "no-table" direct anterior hip resurfacing arthroplasty after a series of cadaver model trials.
This video demonstrates a safe technique for "no-table" direct anterior hip resurfacing arthroplasty by highlighting additional steps compared with conventional total hip arthroplasty, allowing surgeons who have mastered "no-table" direct anterior total hip arthroplasty to easily learn the technique. The advantages of this technique include improved acetabular component positioning, preservation of femoral head vascularity, and shortened recovery time.
The video describes the entire surgical procedure from skin-to-skin, presents a literature review, and reviews outcomes from the authors' institution. Anatomic diagrams and the location of retractors are used to highlight the important aspects of the procedure.
Surgical Steps
1. Skin incision and anterior capsule release
• The tensor fascia lata is split up to the iliac wing, and 20 mm of the tensor fascia lata origin is detached from the iliac wing to attain good visualization of the femoral head.
• Anterior capsule release is initiated posterosuperiorly, well beyond the mid-coronal plane at the level of the joint margin, and extended anteriorly and distally along the fibers of the iliofemoral ligament, down to 1 cm off the intertrochanteric line.
2. Medial capsule release
• The pubofemoral ligament is detached from the femur down to the lesser trochanter, then proximally up the mid-coronal plane, allowing the femoral head to be exposed and the ligamentum teres to be released.
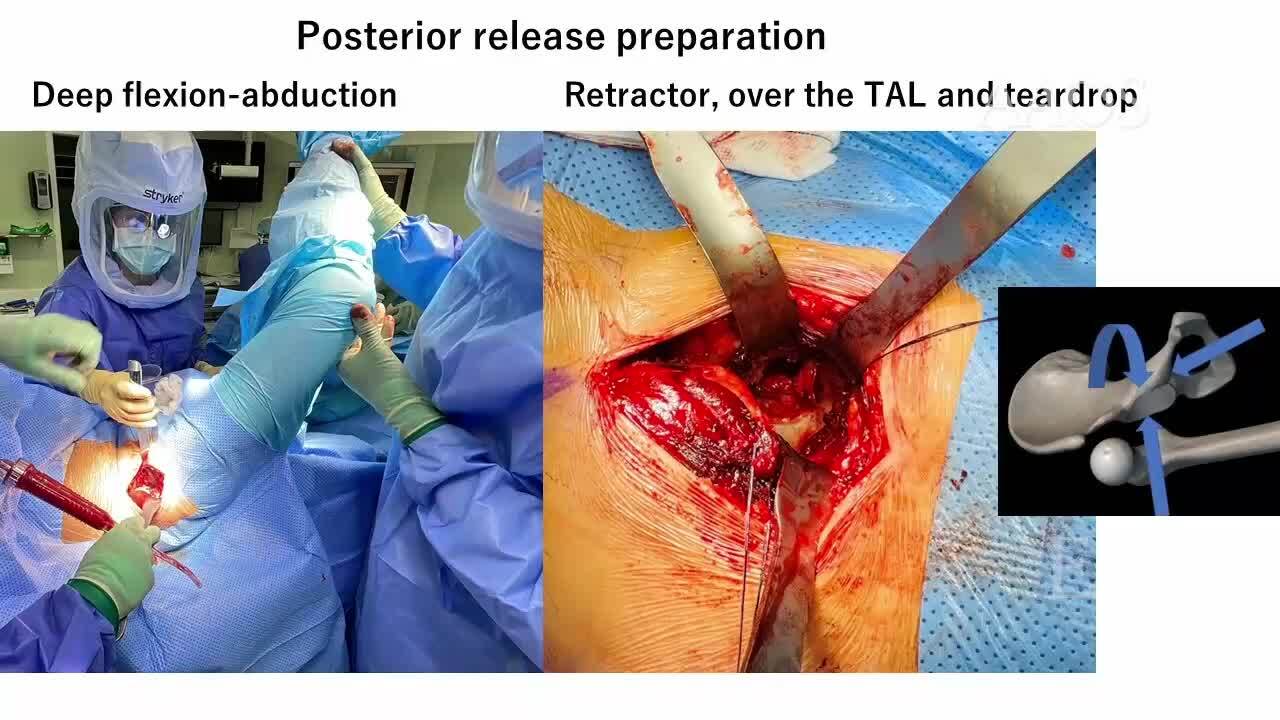
3. Dislocation (posterior release)
• Retractors are placed in the joint space, gently externally rotating the leg and dislocating the hip.
• After dislocation, the hip is flexed to as much as 80°, and posterior capsule release is performed through the zona orbicularis, across the entire ischiofemoral ligament. These steps create space for acetabular reaming and component implantation.
4. Acetabular preparation and component implantation
• The procedure is performed with retractors on the posterior wall, anterior wall, and tear drop.
5. Femoral preparation and component implantation
• Preparation for femoral head exposure is achieved via hip extension.
• The table is "broken", and the leg is slowly dropped to approximately 40° of extension.
• A bone hook is slipped around the back of the femoral neck, gently pulling the femur anteriorly out of the wound. Two large retractors are positioned medially and superiorly to deliver the femur.
• After the femoral head is ready, the guidewire is inserted and checked with a stylus before head preparation and component implantation.
6. Capsule approximation and wound closure
Literature Review and Outcomes
• A study of 555 cases that underwent metal-on-metal hip resurfacing via the direct anterior approach showed a survivorship rate of 95.0% at 5 years postoperatively and 92.5% at 10 years postoperatively. The mean patient age was 49.4 ± 6.9 years, and the mean patient body mass index was 28.1 ± 5.3 kg/m².
• In this series, no substantial complications were reported, except for one femoral neck fracture, which was subsequently converted to total hip arthroplasty.
Conclusion
This video demonstrates that resurfacing via the direct anterior approach is safe and effective if certain measures are taken, specifically splitting the tensor fascia lata up to the iliac wing and performing adequate capsular release, including the entire ischiofemoral ligament and the zona orbicularis.