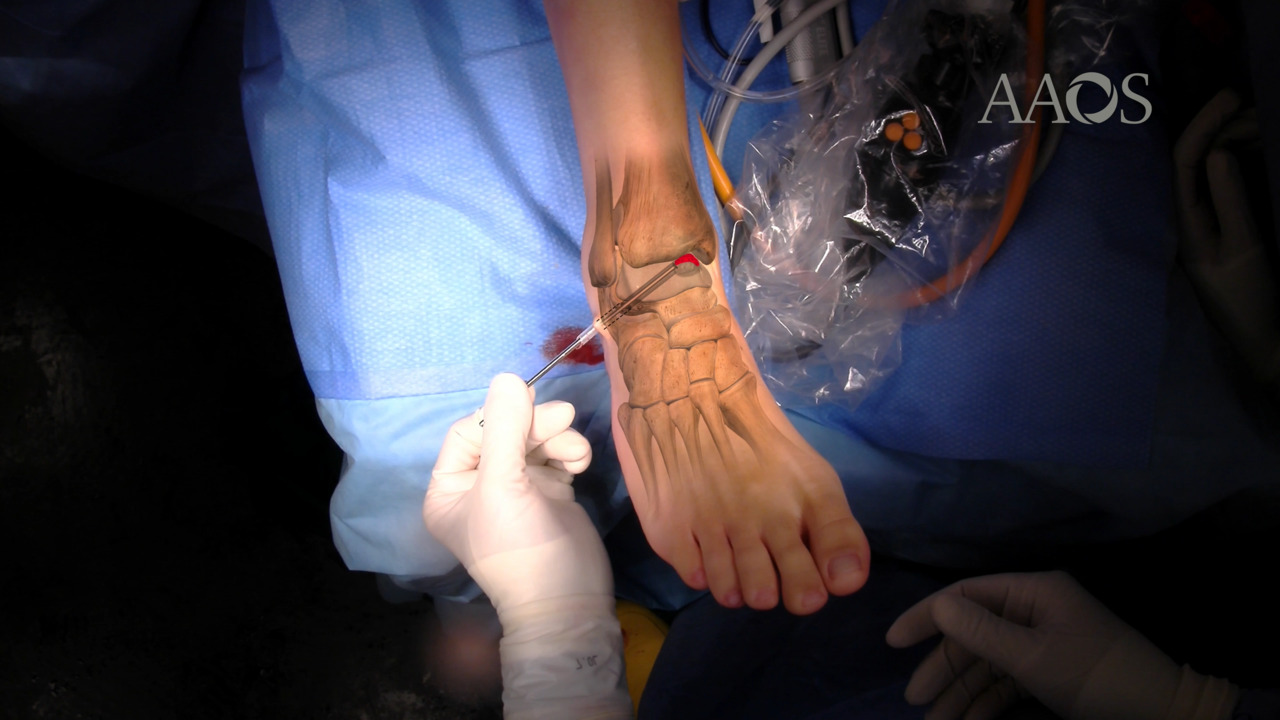
A Retrograde Technique for Ankle Osteochondral Lesion: The Sub-Endochondral Regenerative Treatment (SECRET)
Introduction
Ankle osteochondral lesions (OCL) refer to defects in the cartilage and subchondral bone in the ankle joint. These lesions predominantly affect individuals who lead an active lifestyle, with an incidence rate of 27 cases per 100,000 individuals.
In patients with ankle OCL, the quality of the hyaline cartilage and subchondral bone deteriorate over time, leading to pathologic changes that eventually manifest as ankle arthritis. Therefore, recognition and management of these lesions as early as possible are crucial. Although nonsurgical management has limited effectiveness, many surgical treatment options for ankle OCL have been described; however, the ideal treatment option remains a subject of debate. Bone marrow stimulation techniques are recommended for cystic lesions, with some concerns for the healing potential of the subchondral bone. In patients with a wide osteochondral defect, regenerative solutions are preferred; however, massive chondral débridement usually is required.
This video describes a new surgical technique for the management of chronic OCL of the ankle using bone marrow concentrate on a scaffold and a homologous bone graft positioned via a retrograde approach while preserving healthy hyaline cartilage.
Materials and Methods
This study retrospectively enrolled surgically treated patients with OCL of the talus, either cysts with intact cartilage or wide osteochondral defects. Standard ankle joint standing radiographs and MRIs were obtained to diagnose and evaluate the lesion. A 6-mm tarsal tunnel was retrogradely created toward the lesion to allow for complete sub-endochondral débridement while preserving healthy cartilage. A hyaluronan scaffold soaked with a previously prepared bone marrow concentrate was retrogradely positioned under the cartilage surface, and the tunnel was filled with a homologous bone graft. American Orthopaedic Foot and Ankle Society Scores and visual analog scale scores were evaluated preoperatively and postoperatively, and postoperative radiographs were obtained. At 1-year follow-up MRIs were obtained to evaluate the OCL diameter and bone edema. A T2-weighted mapping MRI of the ankle was obtained to evaluate the water content of the articular cartilage.
Results
A total of 14 patients (9 females, 5 males) with a mean age of 42.3 years (interquartile range [IQR], 24 to 60 years) were treated. The mean follow-up was 28.4 months (range, 12 to 48 months). Of the 14 patients, 12 patients had a medial OCL and two patients had a lateral OCL. The mean preoperative diameter was 11.8 mm (IQR, 9 to 14 mm). In addition to OCL treatment, anterior tibial osteophytes were removed in seven patients, and medial soft-tissue débridement was performed in two patients. The mean American Orthopaedic Foot and Ankle Society Score increased from 53.9 preoperatively (IQR, 33 to 71) to 94 postoperatively (IQR, 86 to 100). The mean visual analog scale score improved from 7.2 preoperatively (IQR, 6 to 10) to 1.3 postoperatively (IQR, 0 to 4). No major complications were reported. MRIs obtained at 1-year follow-up showed a general reduction of the diameter of the OCL and of the surrounding bone edema.
Discussion
The goal of this video is to describe a new cartilage-sparing retrograde technique that may be a viable treatment option for subchondral cysts with intact cartilage and wide osteochondral defects. In patients with a subchondral cyst and an intact cartilage surface, retrograde drilling is the most common treatment option because it does not damage the cartilage. Some concerns exist because of the poor reparative properties of the subchondral bone. In patients with a large OCL and damaged cartilage, various regenerative solutions are available. Even if good improvements in American Orthopaedic Foot and Ankle Society Scores have been reported for all current regenerative techniques, the antegrade approach requires massive débridement of the overlying cartilage.
This novel surgical technique combines various procedures already validated in the literature, intending to exploit their characteristics and improve their effectiveness. An arthroscopic intra-articular view is used to assess the cartilage, remove any loose bodies, and manage concomitant pathology. After assessing the correct indication, a Kirschner wire is retrogradely inserted toward the lesion under fluoroscopic guidance. Large subchondral cysts are associated with poor healing response because of the nonviable subchondral bone and the paucity of mesenchymal stem cells for restoring the lesions. The novelty of this procedure is the hyaluronan scaffold positioned under the cartilage, which may represent an important source of mesenchymal stem cells and promote cell interaction and mechanical stability during the regenerative process, allowing for complete sub-endochondral débridement and restricting chondral removal to only compromised cartilage.
Conclusions
This new procedure was developed to manage large subchondral cysts and wide osteochondral defects, the management of which remains controversial. This technique combines the minimally invasive nature of a retrograde approach with the regenerative properties of biologic scaffolds soaked with bone marrow concentrate, sparing the cartilage and allowing for early recovery. Although additional research is necessary, this novel technique is an intriguing biologic solution with extremely broad applications.