Editor’s note: This is the first in a two-part series. Part two will appear in the July issue and focus on current applications and techniques for nerve blocks and periarticular injections that may be used in a comprehensive approach to pain management.
A comprehensive ‘stewardship’ approach has yielded success at Mayo Clinic
At the AAOS 2019 Annual Meeting Instructional Course Lecture titled “Minimizing Opioids in Total Joint Arthroplasty,” panelists offered strategies for pain management before, during, and after surgery to reduce narcotics use by patients undergoing total hip arthroplasty (THA) and total knee arthroplasty (TKA). Moderator Mark W. Pagnano, MD, of Mayo Clinic in Rochester, Minn., discussed the organization’s “contemporary, multimodal approach,” and Tad M. Mabry, MD, also of Mayo Clinic, discussed contemporary protocols for pain management under the concept of “opioid stewardship.”
Dr. Pagnano noted that a decade ago, surgeons performing TKA and total joint arthroplasty (TJA) tended to operate under the “sick patient model,” by which patients were expected to consume substantial hospital resources and have extended hospital stays. That paradigm has shifted, he said, to the well-patient concept. “We expect that our patients will be optimized prior to surgery and that the procedure will not really throw them off their baseline,” Dr. Pagnano said.
Execution of the well-patient concept involves an approach that seeks to “get ahead and stay ahead” in management of factors beyond pain: “If you are going to do a great job with pain, you have to do a great job with fluid and nausea management,” Dr. Pagnano said.
He described a coordinated pain management strategy that “seamlessly” addresses the pre-, intra-, and postoperative phases. “The multimodal approach aims to stay below the threshold for side effects from any of the medications we are using,” he said. “We want to be preemptive: By staying ahead of pain, we ultimately will limit the total analgesic requirement for the patient.”
Preoperatively, the approach may employ acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs) (e.g., celecoxib), and opioids (e.g., oxycodone) as analgesics, with pregabalin sometimes included. Gabapentin has a sedative effect in older patients and may be avoided. Dexamethasone may be given for antiemetic and analgesic effects. “Orthopaedic surgeons have been traditionally hesitant about its use because of concerns about wound healing or inducing avascular necrosis,” Dr. Pagano said. “But now there is clear and compelling evidence that moderate doses can be beneficial.”
Intraoperatively, spinal anesthesia has the advantages of reduced nausea, less pain in the post-anesthesia care unit (PACU), lower sedation requirement, and no hoarseness or sore throat. Mepivacaine offers a shorter and more predictable half-life, allowing dose to be tailored to predicted surgery time. If general anesthesia is used, total intravenous (IV) anesthesia may be better tolerated than inhalation agents and has a shorter half-life.
Postoperatively, peripheral nerve blocks have the benefit of superior pain relief; however, they are cumbersome and time-consuming and cause a motor block that may slow rehabilitation. Periarticular injections are simple and surgeon-directed, address pain directly at the source, and do not interfere with muscle functions.
After surgery, homegoing medications may include acetaminophen, an NSAID, and an opioid, which Mayo Clinic prescribes, based on guidelines, at a limit of 400 oral morphine equivalents (OMEs) for opioid-naïve TKA or THA patients. Implementation of the guidelines was found to result in fewer opioids prescribed, by about half, with no increase in refills.
“If you want to be delivering the best overall experience for your patients,” Dr. Pagnano said, “you need a deliberate and coordinated plan on how to address pain pre-, intra-, and postoperatively.”
Partnering with patients
Dr. Mabry provided additional detail for executing “opioid stewardship,” which he described as a multidisciplinary approach.
“Realistically, what we are trying to drive toward is a comprehensive protocol involving opioid and nonopioid medication, with an intent to decrease opioid-related impacts and costs and enhance patient health,” he said. “We seek to improve patient care by trying to get the best of both worlds—improved pain control but not telling our patients, ‘You’re just going to have to put up with more pain,’ and thereby decreasing risk of their exposure to opioids.”
As a high-volume category with a high number of prescriptions and high variability, TJA provides a ripe opportunity to practice opioid stewardship, Dr. Mabry said. There is huge variation among providers in the amount of opioids with which patients are discharged. Small changes can lead to large benefits.
Data analysis of discharge prescribing history at Mayo Clinic found that TKA, followed by THA, led all surgical procedures for opioid pills prescribed—with each patient going home with about 100 5 mg oxycodone pills.
The effort to reduce these numbers begins before surgery, with preoperative counseling, Dr. Mabry said. “This should address both patient and caregiver expectations,” he explained. “What is the patient expecting from [the] operation in healing and pain? Our role is to form a realistic expectation. In the past, patients may have had the unreasonable expectation of zero pain after surgery. This is your opportunity to establish a partnership and to make them understand that there are risks with opioids, and we are going to look at ways to minimize their risk.”
He said the physician should try to both inform the patient about opioids and establish that partnership. The effort might involve a conversation with language such as, “On a scale of 10, our target pain score is less than 6. We’d like it to be lower than that, but we want to set a reasonable expectation of wanting your pain to be in the manageable range.”
One issue that must be managed is that of patients already taking opioids. Preoperative use is rather common, with 20 percent to 25 percent of TJA patients having taken opioids in the previous 90 days, although the numbers for daily use are considerably lower. Negative outcomes associated with preoperative, ongoing use include increased pain, lower satisfaction, and higher rates of reoperation and revision.
Thus, an initial action item is to identify those patients. It should be a standard intake question. For such patients, a target reduction of more than 50 percent in daily OMEs should be the goal. For patients taking long-acting opioids and those taking more than 50 OMEs daily, postponement of elective TJA surgery should be considered, Dr. Mabry said.
The pathway
At this point, the opioid-sparing TJA pathway may be mapped, covering the pre-, intra-, and postoperative phases, as well as stays in the PACU and on the specialty floor. Key features of the pathway are that it is multimodal and preemptive; it involves nonopioid agents; and when opioids are prescribed, “start slow and slowly escalate,” Dr. Mabry said.
Before surgery, the preemptive analgesic course consists of acetaminophen 1,000 mg orally, given as an IV dose in the operating room (OR) if a patient cannot take it orally; celecoxib in patients with normal renal function; and, in patients younger than 65 years, pregabalin 150 mg.
For patients at high risk for nausea (e.g., history, female, nonsmoking, general anesthesia), a scopolamine transdermal patch 1.5 mcg may be placed behind the ear.
For TKA, an adductor canal nerve block may be done as a single injection of 0.5 percent bupivacaine 10 mL with epinephrine 1:200,000 plus dexmedetomidine 50 mcg added as a potentiator in appropriate patients.
Intraoperatively, Dr. Mabry said, an opioid-free spinal anesthetic is preferred at Mayo Clinic. The periarticular injection combines ropivacaine, epinephrine, and ketorolac. Antiemetics are ondansetron 4 mg IV and dexamethasone 0.1 mg/kg up to 8 mg IV. Ketamine is administered in divided doses of 10–40 mg between the OR and the PACU.
In the PACU, the analgesic protocol consists of acetaminophen and ketamine routinely, as well as tramadol and then oxycodone/hydromorphone, if needed. “This is a change in philosophy from hitting hard with opioids,” Dr. Mabry said. For breakthrough pain, fentanyl IV is given.
On the specialty floor, the analgesic protocol continues, along with antiemetic therapy.
Discharge is a crucial point in the opioid stewardship pathway. “In absence of perfect data,” Mayo Clinic developed medication guidelines based on four levels of pain:
- level 1: mild pain
- level 2: moderate pain; nonopioids available
- level 3: moderate pain; ± nonopioids unavailable
- level 4: severe pain; nonopioids unavailable
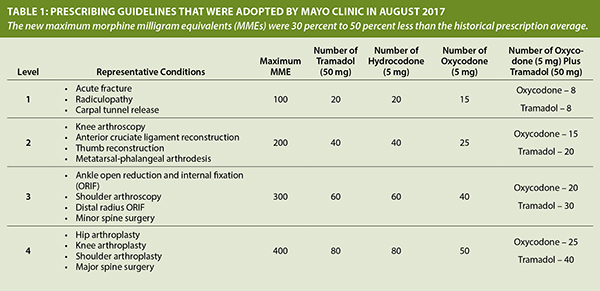
Mayo Clinic created a table of prescribing guidelines matching these levels to various orthopaedic procedures and setting maximum OMEs for each level. TJA, along with shoulder arthroplasty and major spine surgery, is assigned to level 4 (Table 1), which allows for a maximum total OME of 400, which is 30 percent to 50 percent less than the historical average. After the guidelines were adopted, the median number of prescribed OMEs decreased 53 percent (from 675 to 320) and from a range of 450–875 to 188–388.
Along with the guidelines, the protocol set a 12-week limit for involvement of a surgeon in a patient’s pain management; after that, formal handoff is made to an appropriate resource.
After the prescribing guidelines were implemented, Mayo Clinic surveyed consumption by its orthopaedic surgery patients. Based upon the results, the department will be lowering the discharge prescription guidelines: For TKA, the maximum discharge prescription will be 300 OME (60 hydrocodone 5 mg; 40 oxycodone 5 mg) and for THA, it will be 200 OME (40 and 26, respectively).
Terry Stanton is the senior science writer for AAOS Now. He can be reached at tstanton@aaos.org.