In a study of patients who underwent surgical stabilization for glenohumeral instability, 51 percent of patients demonstrated preoperative symptoms consistent with clinical depression (CD), and 24 percent demonstrated symptoms consistent with CD one year after surgery. Furthermore, patients with worse CD symptomatology demonstrated worse pre- and postoperative shoulder function. The researchers defined CD with a previously validated questionnaire used for depression screening.
The study, presented by Richard E. Campbell, BS, a research fellow at the Rothman Orthopaedic Institute, during the American Orthopaedic Society for Sports Medicine Annual Meeting, aimed to identify the prevalence of CD symptoms before and after shoulder stabilization, as well as the relationship between depression and functional outcomes, and to identify predictors of depression symptoms. The investigators hypothesized that patients with preoperative depression symptoms would have significantly worse shoulder function outcomes both pre- and postoperatively.
“Shoulder injuries, especially instability, can have a significant impact on patients’ quality of life,” Mr. Campbell noted. “The majority of our day-to-day activities require pain-free shoulder mobility. Furthermore, the majority of patients with shoulder instability participate in vigorous upper-extremity activities recreationally or vocationally. In addition to quality of life, the inability to adequately participate in these activities affects patients’ self-image. While some patients vocally expressed this decreased quality of life and self-image, we suspected that many other patients are quietly experiencing similar symptoms.”
Mr. Campbell and colleagues undertook the study to quantify and qualify the depression symptoms they were observing in the clinic and to evaluate the relationship between depression symptoms and shoulder function. “Prior evidence suggests that depression symptoms can negatively impact postoperative function after orthopaedic procedures,” Mr. Campbell said. “We wanted to determine if depressed mood was a risk factor for worse postoperative function.”
Methods and results
The study initially enrolled 88 patients preoperatively, and 12 were subsequently excluded because the labrum was not surgically repaired—for a total of 76 patients followed postoperatively.
Potential participants were informed of the intent of the study but were not primed with introductory narratives about the association of musculoskeletal injuries with depression symptoms or the potential for depression symptoms to negatively affect surgical outcomes. To assess depression symptoms, participants completed the 16-item Quick Inventory of Depressive Symptomatology Self-Report (QIDS-SR) questionnaire preoperatively. Total scores on the QIDS range from zero to 27; a score of six or more indicates the presence of CD. Patients with a QIDS-SR score of six or more were assigned to the CD group, whereas patients with QIDS scores less than six were assigned to the non-CD group. The Western Ontario Shoulder Instability Index (WOSI) questionnaire was administered preoperatively to assess shoulder function.
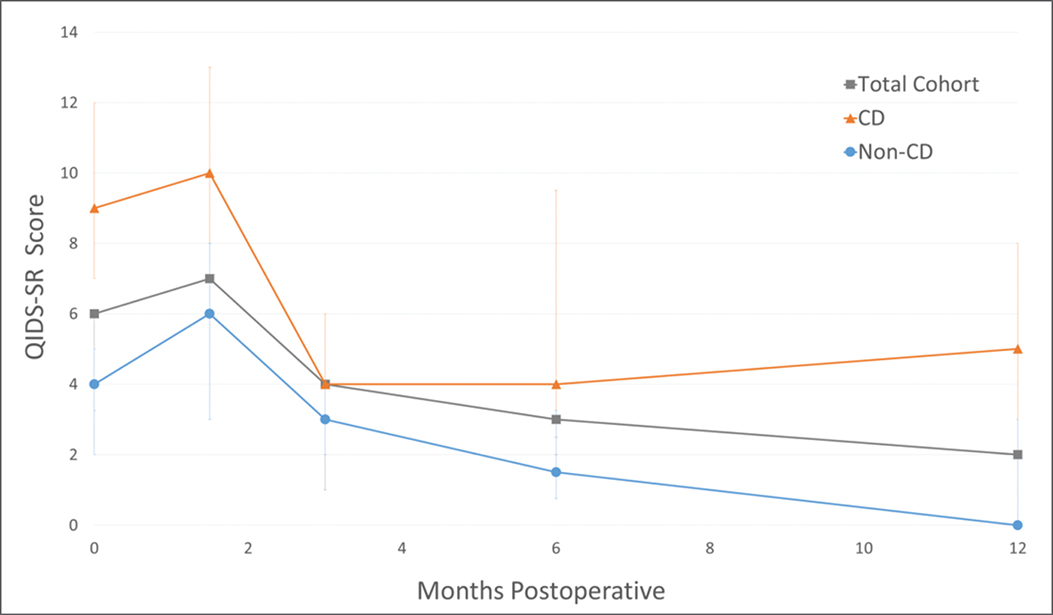
Surgeries were performed by multiple surgeons at one private institution with multiple treatment centers. The prevalence of preoperative CD in the total cohort was 51.3 percent (n = 39), decreasing to 23.7 percent (n = 14/59) at one-year follow-up. QIDS-SR scores and CD prevalence at all timepoints are displayed in Tables 1 and 2 and Fig. 1.
The CD cohort had worse preoperative total WOSI scores than the non-CD cohort. There was a weak correlation between worse depression symptoms and worse shoulder function. The CD cohort demonstrated worse one-year postoperative WOSI scores than the non-CD cohort. At one year postoperatively, worse preoperative depression symptoms correlated with worse shoulder function. Preoperative shoulder function did not correlate with postoperative shoulder function.
“We were surprised by the lack of significant correlation between worse preoperative shoulder function and worse postoperative shoulder function,” Mr. Campbell commented. “This was unusual, as preoperative function is a common indicator of postoperative function. However, this finding helped shed light on the relationship between preoperative depression and postoperative shoulder function. The fact that preoperative shoulder function did not correlate with postoperative shoulder function, while preoperative depression did correlate with worse postoperative shoulder function, indicates that the relationship between depression symptoms and postoperative shoulder function is not mediated by preoperative shoulder function.”
The study authors wrote, “The prevalence of depression among patients with glenohumeral instability is concerning.” The finding that more than half of the cohort had CD symptomology preoperatively is concerning, “when compared to the 8.1 percent prevalence of adult depression in the United States during 2013 to 2016,” the researchers added. They noted that although other studies have reported alarming rates of depression among patients with upper-extremity injuries, “The use of different methodologies prevents direct comparisons.” The prevalence of depression among patients with rotator cuff tears ranges from 12.8 percent to 26.2 percent when measured with the Hospital Anxiety and Depression Scale (HADS). Furthermore, 36 percent of patients with lateral epicondylitis of the elbow report depression symptoms on the HADS measure. In contrast, one study by Koorevaar et al., reported depression symptoms in 3 percent of patients with shoulder instability and 8 percent of patients with rotator cuff rupture.
In discussing their finding that patients in the CD cohort had worse preoperative shoulder function and worse shoulder function one year postoperatively, the authors of Mr. Campbell’s study observed: “Both groups equally improved over time; thus, while depression symptoms were associated with worse shoulder function, depression symptoms did not affect the utility of surgical stabilization as a treatment for glenohumeral instability.”
Function and depression: a link?
The authors observed that although their findings show a clear relationship between depression and shoulder function, the causative relationship between the two factors is unclear, and the relationship may be mediated by another variable. “The high prevalence of CD in patients with shoulder instability indicates that shoulder impairment likely leads to CD; therefore, worse shoulder symptoms may lead to worse depression symptoms,” they wrote. “However, this is opposed by the lack of correlation between pre- and postoperative shoulder function. If shoulder impairment mediated the relationship between depression and shoulder function pre- and postoperatively, worse preoperative shoulder function would correlate with worse postoperative shoulder function. Alternatively, depression symptoms may cause inferior shoulder function in patients with shoulder instability. The correlation between pre- and postoperative depression symptoms indicates that the same psychosocial factors influencing preoperative depression may continue to affect patients postoperatively, thus mediating postoperative function.”
Orthopaedic surgeons should consider screening patients who present with debilitating musculoskeletal injuries using standardized methods (QIDS-SR, HADS, etc.) and should refer patients who endorse CD symptoms to a psychiatrist or psychologist for evaluation, the authors advised. Mr. Campbell said that one approach would be for orthopaedic surgeons to implement validated CD questionnaires into their practice. “This could be done at multiple levels,” he said. “The first would be to incorporate a brief depression screen such as the Patient Health Questionnaire-9 into new patient or new problem intake forms. Another option would be to ask medical assistants or nursing staff to administer these questionnaires when placing patients in rooms. Finally, physicians can mention the effect of mental health on postoperative outcomes during preoperative counseling and screen patients at that time.”
Commenting on the study’s limitations, Mr. Campbell said: “Unfortunately, due to the design of our study, we cannot make firm conclusions about the causative relationship between depression symptoms and shoulder function. Another limitation is that patients lost to follow-up demonstrated worse preoperative depression scores. Therefore, the incidence of postoperative CD may be greater.”
Mr. Campbell’s coauthors of “Prevalence of Clinical Depression Among Patients After Shoulder Stabilization Repair” are Danielle G. Weekes, MD; Weilong J. Shi, MD; Nicholas Giunta; Matthew D. Pepe, MD; Bradford Tucker, MD; Michael Ciccotti, MD; William Emper, MD; Kevin B. Freedman, MD; and Fotios P. Tjoumakaris, MD.
Terry Stanton is the senior science writer for AAOS Now. He can be reached at tstanton@aaos.org.

