Patients undergoing total joint arthroplasty (TJA) of the hip or knee reported higher satisfaction and better compliance with both pre- and postoperative protocols with the use of mobile applications, compared to standard care, according to a systematic review and meta-analysis, to be presented today. The findings suggest that apps are low-cost interventions that can help ensure high-quality care for TJA patients.
Rubén Monárrez, MD, a postgraduate year-1 orthopaedic resident at the Rubin Institute for Advanced Orthopedics at Sinai Hospital of Baltimore, will present the study.
“Smartphones have become ubiquitous devices, and other fields of medicine are leveraging their power to improve patient care,” Dr. Monárrez told AAOS Now Daily Edition. “Arthroplasty is a prime intervention to apply mobile applications because it represents a relatively short, finite episode of care that is highly dependent on patient participation.”
The researchers scanned Embase, Medline, and Web of Science databases for studies that compared patient experiences post-TJA, compliance with pre- and postoperative protocols, and procedure-associated complications with standard care or with the use of patient-facing mobile applications.
The analysis included a wide variety of mobile applications, Dr. Monárrez explained. “Most provided real-time reminders to arthroplasty patients, others provided educational videos and information, and some offered a direct connection with healthcare providers or automated sys¬tems for questions that arose throughout the surgical process,” he said.
Patient satisfaction was reported as continuous values according to a variety of tools across the studies, so satisfaction was analyzed with Hedge’s g. The researchers also evaluated pooled odds ratios (ORs) for patient adherence.
Twelve studies, involving a total of 9,521 patients, met inclusion criteria. Average patient age was 60 years.
Half the studies reported that mobile applications improved patients’ experiences after TJA. Hedge’s g analysis revealed an effect size of 1.64 (95 percent confidence interval [CI] 0.90–2.37; P <0.001) in favor of mobile applications increasing patient satisfaction. The improvements were driven largely by improvements in communication, the authors noted. “We were surprised to find that the largely older patient cohorts were very receptive to using mobile applications to interact with their healthcare team,” Dr. Monárrez said.
Six studies reported large improvements in compliance, the researchers added. The pooled OR for adherence was 4.57, representing increased likelihood of compliance with mobile applications compared to standard care (95 percent CI 1.66–12.62; P <0.001). Another two studies suggested that use of a mobile application could reduce healthcare resource utilization, finding a lower incidence of unscheduled office and emergency department visits with the use of mobile applications.
“With evolving reimbursement policies linked to surgical outcomes paired with the exponentially increasing volume of TJA performed in the United States, innovative ways to efficiently deliver high-quality care at low cost are in demand,” the authors observed. Mobile applications could be a tool to accomplish these goals. However, although the results of the meta-analysis suggest improvement across patient outcomes, “We are in need of well-developed, randomized, controlled trials free of bias to further quantify the impact mobile applications have on arthroplasty patients,” Dr. Monárrez said. In addition, the analysis was not designed to compare patient satisfaction rates among the different mobile apps studied.
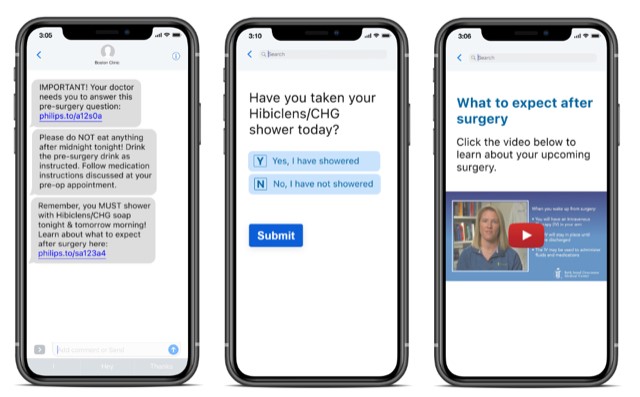
The findings also inspired Dr. Monárrez and his colleagues to create their own mobile application to help improve patient experiences with TJA (Fig. 1). “We partnered with local developers to implement and study this application at our hospital. We are currently analyzing our results and will be publishing them soon.”
Dr. Monárrez’s coauthors of “The Effect of Mobile Applications on Patient Compliance and Outcomes following Total Joint Arthroplasty of the Hip and Knee: A Systematic Review and Meta-Analysis” are Amin Mohamadi, MD, MPH; Jacob M. Drew, MD; and Ayesha Abdeen, MD.
Ariel DeMaio is the managing editor of AAOS Now. She can be reached at ademaio@aaos.org.