A study exploring the role of cultures and outcomes among diaphyseal tibia nonunions in both presumed septic and aseptic nonunions found that nearly one-third of patients with tibia nonunion had positive intraoperative cultures. Evidence supporting a benefit of antibiotics for nonunion patients remains inconclusive.
In the study, presented yesterday by Malcolm DeBaun, MD, culture-positive patients were more likely to have persistent nonunion after repair, reoperation, and readmission to the hospital compared to aseptic nonunions. However, the clinical course of patients with negative cultures obtained in nonunion surgery was similar to those patients with low clinical suspicion for infection and surprise positive cultures.
The findings demonstrate that “the controversy in intraoperative cultures obtained at the time of diaphyseal tibia nonunion repair remains,” Dr. DeBaun, of Duke University, told AAOS Now Daily Edition. He noted that intraoperative culture of presumed septic nonunion based upon elevated inflammatory markers or signs of infection demonstrates relevant prognostic value, but “the clinical benefit of adjunctive antibiotic treatment indicated by positive culture results remains elusive.”
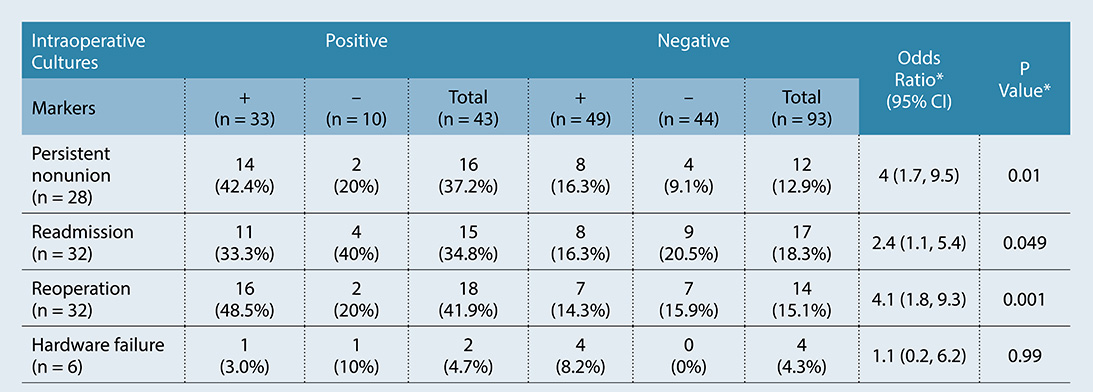
The preliminary analysis included 191 primary tibia nonunions with complete preoperative inflammatory markers, including 136 patients (71 percent) who had intraoperative cultures taken (Table 1). Median length of follow-up was 19.6 months. Thirty-two percent of patients with intraoperative cultures (n = 43) had positive cultures and 7 percent (n = 10) had surprise positive cultures, defined as negative preoperative inflammatory markers with positive cultures. Patients with positive culture results were more likely than those with negative culture results to have persistent nonunion after repair (37 percent versus 13 percent; P <0.01) and to require readmission for related complications (35 percent versus 18 percent;>P = 0.05).
Patients with positive cultures also had increased risk of persistent nonunion (P <0.01) and readmission (>P = 0.04) compared to patients with negative cultures. Patients with positive cultures (presumed septic and surprise positive) demonstrated more persistent nonunions (37 percent versus 7 percent; P <0.01) and increased readmission rates (35 percent versus 7 percent;>P <0.01) compared with the group with no culture taken. patients with surprise positive cultures, even when treated, had similar complication rates to those with no cultures taken, with the exception of higher readmission rates (40 percent versus 7.4 percent;>P = 0.035). This group also had negative preoperative inflammatory markers.
The authors noted that routine intraoperative culture at the time of nonunion repair is not universally recommended. Proponents of taking routine cultures cite meaningful rates of positive cultures in patients undergoing revision fracture surgery, at 20 percent, even in the setting of low clinical suspicion. From this perspective, patients with positive cultures would then be administered targeted antibiotics postoperatively. “Despite the theoretical benefit, evidence supporting improved clinical outcomes in surgically repaired septic nonunion patients treated with prolonged antibiotics remains underwhelming, especially in patients with low pretest probability of infection,” the researchers wrote.
Dr. DeBaun said that his clinical impression leads him to believe that obtaining routine intraoperative cultures at the time of nonunion repair can, at the very least, inform prognosis. When the suspicion for infection (elevated inflammatory markers and/or clinical signs of infection) is high, he said, thorough surgical debridement is recommended, with a staged approach to the nonunion repair involving a medullary antibiotic-eluting implant before definitive repair. “Targeted systemic antibiotic therapy may not be beneficial in all patients with tibia nonunion whose cultures have a positive result,” Dr. DeBaun said.
The findings of the study, he said, support the merit of determining which patients diagnosed with septic nonunion would benefit from targeted antibiotic therapy. “The additive benefit from systemic antibiotic treatment may be negligible in some patients and is not without the associated medical risks,” he said, adding that “establishing refined indications for intraoperative culture during nonunion repair may prevent spurious results that confound management decisions.”
The authors noted that the study results do not establish that using culture results to inform targeted antibiotic administration improves clinically relevant outcomes. “Although this study was underpowered to demonstrate equivalence, we did not detect a difference in the surgical complication profile between culture-positive patients treated with and without systemic antibiotics,” they wrote. “Surgical debridement, whether deliberate or resulting from routine medullary reaming in exchange nailing, may be sufficient to definitively treat infection in septic nonunions.”
Addressing the study’s limitations, Dr. DeBaun said: “This was a study of outcomes from a heterogeneous group of surgeons across multiple institutions with differing nonunion repair strategies and thresholds for obtaining intraoperative cultures. However, the results justify randomized prospective investigation to clarify the indication and utility of intraoperative culture in tibia nonunion repair surgery.”
Dr. DeBaun’s coauthors of “The Role of Cultures in Diaphyseal Tibia Nonunions: A Multicenter Study” are Cara Lai, MD; Michael James Chen, MD; Joseph R. Hsu, MD; and Michael J. Gardner, MD, and the EMIT Nonunion study group.
Terry Stanton is the senior medical writer for AAOS Now.