
Modern methods to enhance sports performance incorporate a variety of techniques and technologies. The purpose of this article is to explore some of the most prominent and useful tools available and briefly outline their roles in performance enhancement. These devices are available and utilized at most training facilities where high-level athletes are trained and are becoming increasingly available in physical therapy locations across the United States.
Underwater and antigravity treadmills
Underwater (Fig. 1) and antigravity treadmills allow for rehabilitation or training at sub-physiologic loads by reducing bodyweight conditions. When used in postoperative rehabilitation, these devices allow for earlier return to running prior to when the athlete is ready for full weightbearing. For example, Saxena and Granot compared return to running in patients who did and did not use an antigravity treadmill in the postoperative rehabilitation of Achilles tendon rupture. They found that those who utilized an antigravity treadmill in their recovery returned to running at 70 percent of their bodyweight 6 weeks earlier than the control group returned to ground running. The antigravity group also returned to ground running 2 weeks sooner than the control group. This demonstrates the ability for patients to work on kinematics earlier and build a competitive edge by returning to activities more quickly.
These treadmills also can be used as performance-enhancement tools in uninjured athletes, as they leverage the principles of hydrostatic pressure to facilitate blood and lymphatic flow during recovery activities. Underwater treadmills have the added benefit of resistance from the water, which helps build strength throughout the entire arc of motion during running. Additionally, underwater treadmills allow for natural running mechanics.
Antigravity treadmills are sealed at the waist and use a pressurized chamber surrounding the lower extremities to reduce bodyweight. Many allow for reduced weightbearing loads, ranging from 20 percent bodyweight to full weightbearing. Distance runners and multi-sport athletes can benefit from their use, as they can train at a 10 to 15 percent decrease in bodyweight, thereby significantly lowering the cumulative ground reaction forces associated with over-ground run training volume.
These devices are particularly useful to accelerate rehabilitation by allowing athletes to quickly progress to full running. This allows athletes to bypass the typical run-walk cycle, which has been used historically to reduce the load on an injured limb. The progressive loading achievable with these devices has demonstrated value in postoperative anterior cruciate ligament reconstruction rehabilitation, stress fractures or soft-tissue injuries of the lower extremities, and lumbar disk herniation rehabilitation.
GPS tracking devices
Increasingly small and portable GPS devices have begun to be implemented in sport. Athletes can wear a vest with a GPS accelerometer positioned on the back between the scapulae near the cervico-thoracic junction. This allows for measurement of performance metrics such as total distance, maximum velocity, position on pitch or field, ground impacts, and acceleration rate.
Quantitative information is obtained to monitor player workload and recovery. In the uninjured athlete, this information can be a valuable tool for coaches to plan athlete-specific playing time and substitutions through the use of an objective measure of acute to chronic workload, which previously had to be calculated by utilizing a subjective rate of perceived exertion (RPE) calculation (e.g., RPE value [1–10 scale] x number of minutes of activity = subjective player load). This information can be compared against individual baseline and position-matched controls to make informed decisions on player readiness and guide long-term athletic development. Specific metrics often used for this purpose are total player load, total distance covered, number of explosive efforts, maximum velocity attained, number of high-speed repetitions, and total high-speed distance in a session. Together, these give a sense of an athlete’s ability to achieve and maintain high physiologic loads.
Force plates
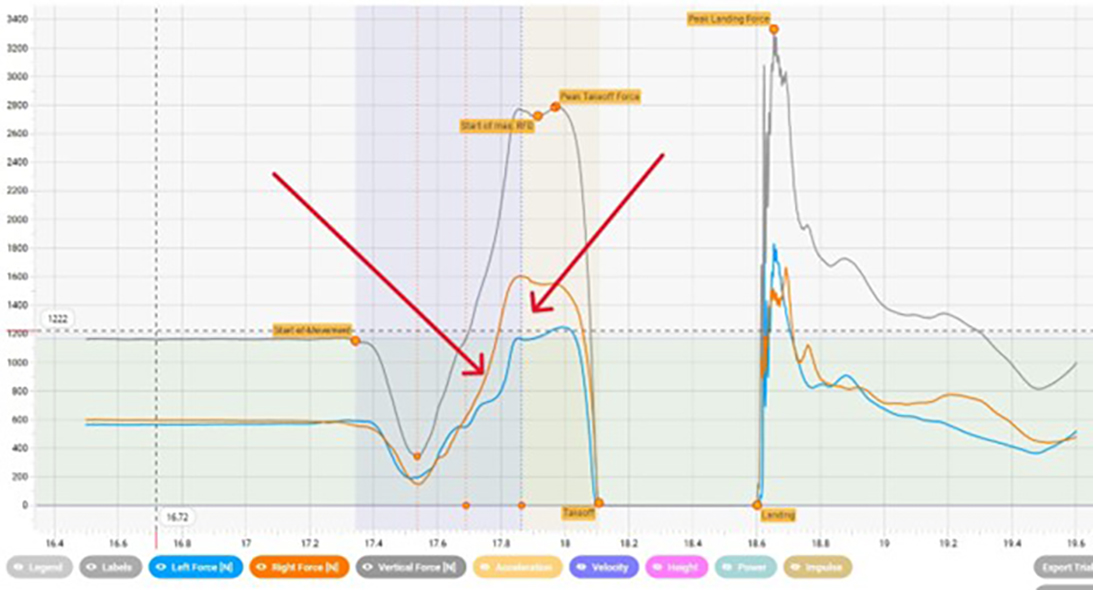
Force plates are devices equipped with mechanical sensors that are placed under an athlete’s feet to quantify and map ground reactive forces during exercises and movements. The countermovement jump (Fig. 2) and drop jump are two tests commonly used with force plates. These tests combined with an isometric mid-thigh pull can help quantify an athlete’s dynamic strength index. In the countermovement jump test, an athlete squats and performs a vertical jump as high as they are able. This allows for measurement of lower-limb power development and asymmetry. In the drop jump test, an athlete stands on a raised platform behind the force plate, drops off onto the force plate, and immediately propels themselves into a jump. This allows measurement of limb symmetry and reactive strength and jump height, which can be utilized to monitor fatigue and assess physiologic response to training.
These data are mapped, quantified, trended, and displayed for the physical therapist and physician to interpret. As with the GPS system, the data also may be used to identify additional areas for training to enhance performance.
Conclusion
Modern methods to enhance sports performance and recovery utilize multiple technologies to monitor an athlete’s physiologic training response and tailor their program accordingly. Integration of these devices into an exercise program can provide the physician and physical therapist with objective, quantifiable data to help guide patient care.
David Heath, MD, is a current fellow in orthopaedic sports medicine at University of California, Los Angeles (UCLA). This fall, he will start a new position as an assistant professor in orthopaedic surgery at University of Texas Health San Antonio.
Jeremy Vail, PT, SCS, OCS, ATC, is director of rehabilitation in the Department of Intercollegiate Athletics at UCLA.
Thomas Kremen, MD, FAAOS, is an assistant professor of orthopaedic surgery at the David Geffen School of Medicine at UCLA, specializing in orthopaedic sports medicine. Dr. Kremen is a team physician for UCLA intercollegiate athletics, the associate team physician for the Los Angeles Lakers, and the chair of sports medicine for USA Swimming.
David McAllister, MD, FAAOS, is a professor of orthopaedic surgery and chief of sports medicine at the David Geffen School of Medicine at UCLA. He is also the head team physician for UCLA Athletics.
Reference
- Saxena A, Granot A: Use of an anti-gravity treadmill in the rehabilitation of the operated Achilles tendon: a pilot study. J Foot Ankle Surg 2011;50(5):558-61.
- Raghu SL, Conners RT, Kang CK, et al: Kinematic analysis of gait in an underwater treadmill using land-based Vicon T 40s motion capture cameras arranged externally. J Biomech 2021;124:110553.
- Vincent HK, Madsen A, Vincent KR: Role of antigravity training in rehabilitation and return to sport after running injuries. Arthrosc Sports Med Rehabil 2022;4(1):e141-9.