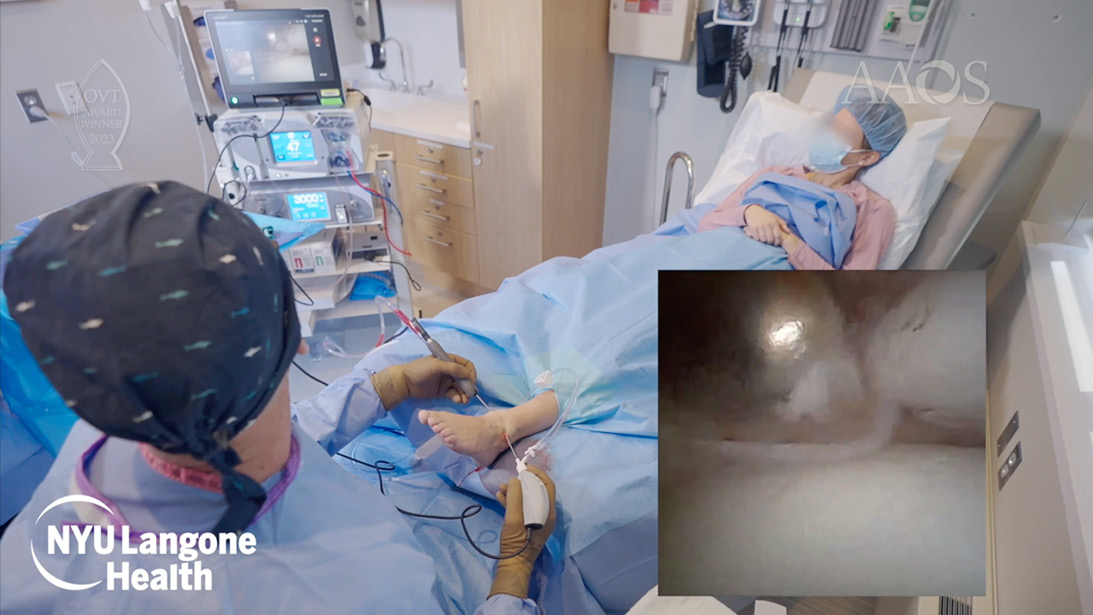
For patients with persistent ankle or knee pain, evaluation no longer always requires a trip to the operating room. In-office needle arthroscopy (IONA) enables real-time visualization and treatment of select joint pathologies under local anesthesia, reducing procedural burden while maintaining the image quality needed for clinical decision making (Figure 1).
Advances in visualization and instrumentation have broadened the utility of IONA for both diagnostic and therapeutic purposes. When applied thoughtfully, the technique can support real-time decision-making and streamline care for a variety of joint conditions.
Ankle impingement is significantly improved with IONA
Ankle impingement is a common condition in athletes, arising when soft tissue or bony structures are repeatedly compressed at the anterior or posterior ankle joint during motion. Anterior ankle impingement is frequently seen in sports that involve cutting, pivoting, or rapid deceleration, such as soccer and football. Colasanti and colleagues found that patients who underwent IONA for anterior ankle impingement experienced clinically meaningful improvements in pain and function, as demonstrated by improved Foot and Ankle Outcome Scores (FAOS) and Patient-Reported Outcomes Measurement Information System (PROMIS) scores.
Beyond its therapeutic role, IONA also demonstrated markedly superior diagnostic accuracy (94%) compared with MRI (55%), underscoring its effectiveness in identifying intra-articular pathologies that otherwise may have been missed. The enhanced visualization during the procedure allows surgeons to directly assess the impingement in real time, providing further diagnostic clarity to target treatment for the patient. Furthermore, patients returned to work within just two days, with 96% returning to sports by four-week follow-up.
Posterior ankle impingement tends to occur in athletes who engage in sports conducive to forced plantarflexion, such as dancers, gymnasts, and soccer players. These types of athletes typically report pain from their posterior ankle impingement when pushing off the ground, jumping, or landing. Mercer and colleagues found that patients who underwent IONA for posterior ankle impingement demonstrated significant improvement in FAOS, with no associated complications among the 10 patients who underwent the procedure. Patients returned to sports in four weeks and were able to return to work in three days.
IONA is useful for evaluating and treating osteochondral lesions of the talus
Osteochondral lesions of the talus (OLTs) involve damage to the articular cartilage and often subchondral bone in the talus. OLTs are typically associated with ankle trauma or repetitive microtrauma, with most cases occurring in patients between 20 and 40 years of age. Treatment options include marrow stimulation, grafting with cancellous bone, and various scaffolds.
IONA has become a useful tool in the evaluation and treatment of OLTs. Walinga and colleagues found that IONA reliably identified high-quality reparative cartilage postoperatively. If a secondary therapeutic intervention is required, the procedure can be performed via IONA. IONA can also be used to deliver extracellular matrix cartilage allograft (ECMA) after bone marrow stimulation. Patients who undergo bone marrow stimulation augmented with ECMA demonstrate greater defect fill on MRI and significant improvements in patient-reported outcomes, and the procedure is associated with low complication and failure rates.
Other foot and ankle pathologies benefit from IONA
IONA has also demonstrated utility across a variety of other foot and ankle pathologies, including hallux rigidus, subtalar joint impingement, lateral ankle repair, and treatment of tendon disorders, all with excellent patient-reported outcome measures, return-to-play times, and low complication rates. For example, the procedure can allow for direct visualization of the posterior tibial tendon (PTT) to identify potential concomitant pathologies that were missed on imaging. A similar benefit exists for patients with peroneal tendon pathology, as IONA allows for accurate assessment and targeted intervention. The minimally invasive nature of the procedure, combined with the opportunity for patients to remain awake and actively engaged with the surgeon, makes IONA a promising treatment option for a wide range of foot- and ankle-related sports injuries.
Applications in knee pathologies
In the knee, IONA can function as both a diagnostic and therapeutic modality for common sports-related pathologies while avoiding an operating room setting and general anesthesia. For meniscal pathology, standard anterolateral and anteromedial portals can be created in the knee to allow real-time investigation, with careful assessment for degenerative changes, fraying, or mechanical instability of the meniscal tissue. When indicated, a 3.8-mm shaver can be used to debride unstable meniscal tissue or surrounding hypertrophic synovium. At this time, the anterior cruciate ligament (ACL) and posterior cruciate ligament (PCL) are systematically probed to confirm structural integrity. To optimize visualization of the lateral compartment, the knee is placed in a figure-of-4 position. The lateral meniscus is then evaluated diagnostically via needle arthroscopy, with focal pathology addressed therapeutically when appropriate. Depending on tear morphology and tissue quality, treatment may include in-office partial meniscectomy or all-inside meniscal repair.
For patellofemoral pain associated with lateral maltracking, an IONA technique can be used to perform a lateral parapatellar retinacular release in appropriately selected patients. Concomitantly, chondroplasty can be performed to address areas of unstable or fibrillated articular cartilage. The lateral gutter may also be accessed to allow for selective synovectomy, facilitating excision of inflamed synovial tissue within the lateral compartment. Finally, for focal chondral or osteochondral lesions, IONA can be used to perform chondroplasty and bone marrow stimulation, followed by the application of a cartilage allograft extracellular matrix, in addition to biologic augmentation. Similar to in-office procedures performed for foot and ankle pathologies, patients undergoing IONA for knee conditions can immediately bear weight following the procedure, with physical therapy typically initiated seven to 10 days following the procedure when clinically indicated. In terms of the safety of the procedure, McMillan and colleagues reported no major complications across 1,419 knee and shoulder IONA, with a minor complication rate of 1.6% for knees.
Conclusion
In-office needle arthroscopy is increasingly redefining how lower extremity joint pathology can be evaluated and treated. Its application across the foot, ankle, and knee highlights the potential for a minimally invasive, clinic-based approach to streamline care while preserving the visualization necessary for confident clinical decision making. While larger prospective studies examining patient-reported outcomes, return-to-sports timelines, and complication rates are needed to further define best practices, early experience suggests a growing role for IONA in modern orthopaedic care. As experience and evidence evolve, IONA has the potential not only to complement existing arthroscopic techniques but also to reshape how and where select lower-extremity conditions are managed.
Jared Rubin, BA, is a medical student at the University of Illinois College of Medicine in Chicago and is currently completing a dedicated research year at NYU Langone Health under the mentorship of Dr. John G. Kennedy.
John G. Kennedy, MD, FRCS (Orth), is a professor of orthopaedic surgery and the chief of division of Foot & Ankle Surgery at NYU Langone Health. He is a co-founder of the International Society for Cartilage Repair of the Ankle and is a pioneer in the realm of in-office needle arthroscopy.
More on IONA
The AAOS OVT video “In-Office Needle Arthroscopy for Treatment of Anterior Ankle Impingement” provides an overview and case presentation on the use of in-office nano-arthroscopy for the management of anterior ankle impingement. View here.
References
- Gianakos AL, Kennedy JG. In-office needle arthroscopy: indications, surgical techniques, tips, and tricks. JAAOS Glob Res Rev. 2024;8(2). doi:10.5435/JAAOSGlobal-D-23-00124
- Colasanti CA, Mercer NP, Garcia JV, Kerkhoffs GMMJ, Kennedy JG. In-office needle arthroscopy for the treatment of anterior ankle impingement yields high patient satisfaction with high rates of return to work and sport. Arthroscopy. 2022;38(4):1302-1311. doi:10.1016/j.arthro.2021.09.016
- Mercer NP, Samsonov AP, Dankert JF, et al. Improved clinical outcomes and patient satisfaction of in-office needle arthroscopy for the treatment of posterior ankle impingement. Arthrosc Sports Med Rehabil. 2022;4(2):e629-e638. doi:10.1016/j.asmr.2021.12.004
- Walinga AB, Butler J, Dahmen J, et al. Second-look needle arthroscopy after prior surgical treatment for cartilage lesions of the ankle: the Amsterdam and New York City perspectives. Cartilage. Published online December 16, 2024. 19476035241306550. doi:10.1177/19476035241306550
- Shimozono Y, Williamson ERC, Mercer NP, et al. Use of extracellular matrix cartilage allograft may improve infill of the defects in bone marrow stimulation for osteochondral lesions of the talus. Arthroscopy. 2021;37(7):2262-2269. doi:10.1016/j.arthro.2021.03.032
- Butler J, Hartman H, Dhilllon R, et al. Outcomes following the use of extracellular matrix cartilage allograft for the management of osteochondral lesions of the talus: a systematic review. Cureus. 2024;16(6):e62044. doi:10.7759/cureus.62044
- Kirschner N, Owusu-Sarpong S, Neal WHE, et al. In-office needle arthroscopy with meniscal repair for meniscal lesions of the knee. Arthrosc Tech. 2023;12(10):e1821-e1826. doi:10.1016/j.eats.2023.06.013
- McMillan S, Chhabra A, Hassebrock JD, Ford E, Amin NH. Risks and complications associated with intra-articular arthroscopy of the knee and shoulder in an office setting. Orthopaedic Journal of Sports Medicine. 2019;7(9):2325967119869846. doi:10.1177/2325967119869846