Over the last several years, we have heard about the many successes of wide-awake surgery and the ongoing shift from the operating room to the office surgical suite. As we continue to make and celebrate progress, though, two things remain clear: In-office cases remain a minority, and those who share their successes mainly focus on what they can do and how effective in-office surgery is.
Very few surgeons address how to get started with in-office surgery in the first place. For those who want to do so, answering these questions is important: How do we build buy-in? From stakeholders with a variety of perspectives and biases? Who are the individuals who can support or sabotage our efforts to start in-office surgery?
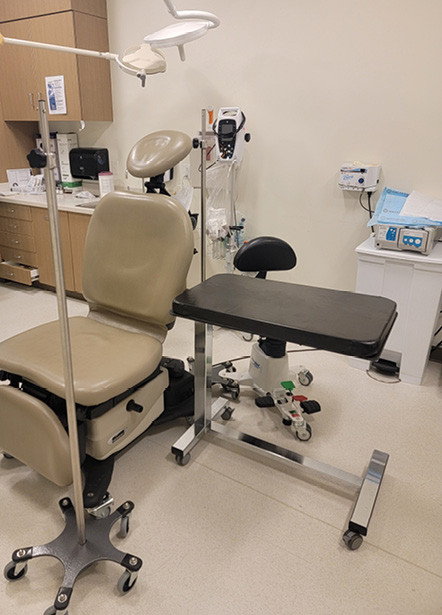
Launching an in-office surgery program is less about buying equipment and more about changing culture. The physical requirements of an office‑based operating suite are modest compared with a traditional operating room and can often be accommodated within existing clinic space (Figure 1). An intentional, staged approach is the only way to make it safe and sustainable, particularly when you are part of a system where several parties must sign off before anything gets done.
Your first job is to articulate why office-based surgery is better for patients, surgeons, and the system. If you believe wide awake, local anesthesia, with no tourniquet (WALANT) is a huge success, in-office surgery is WALANT 2.0. It allows patients to avoid the many perioperative hurdles that are unwarranted yet entrenched within operating room surgery, including routine preoperative assessments and testing, gowning, IV placement, physiologic monitoring, and fasting requirements. Health systems and payers, meanwhile, see lower expenses, reduced staffing needs, and freed-up OR capacity for more demanding cases. If you cannot tell that story in two or three clear sentences to each stakeholder, you are not ready to launch.
But there is a catch: One message does not fit all.
Build buy-in before building rooms
Different stakeholders come with different interests and risk aversions. Marketing principles dictate that, to sell a product, one must identify the various consumer archetypes and satisfy their needs. As a future in-office surgeon, you must map your stakeholder archetypes and engage them deliberately: the influencer, the controller, the buyer, and the potential saboteur. In this sense, the best launch strategy is political before it is procedural, and ignoring the archetypes’ perspectives invites neglect and even obstruction.
Start by leveraging the benefits to patients (i.e., end users) and pre-promote the idea of in-office surgery. Who would want to spend half a day in the hospital for a seven-minute procedure? Why subject patients to unwarranted perioperative processes meant for joint replacement and spine surgery? Do we really need an IV-line, monitor, and sequential compression device other than to satisfy OR policy?
Find your influencers. These are your champions, the surgeon leaders you trust. While they would not necessarily perform in-office surgery, they appreciate innovation and see the potential. Your champions may even find a secondary benefit: They will appreciate the availability of a procedural suite they can use for a quick stop and avoid waiting for their add-on on a Friday afternoon.
Engage those who are in control and who hold the keys to your success. Treat infection control and compliance as allies, not obstacles; ask directly what they need to see to support an office suite. Be familiar with the laws and regulations that guide what they do. They are not there to make your life difficult — they want to keep the organization out of trouble. And although they do not truly understand surgery, they do understand the Centers for Medicare & Medicaid Services (CMS) and The Joint Commission (formerly Joint Commission on Accreditation of Healthcare Organizations, JCAHO).
Sit down with the administration, your buyer, the C-suite people who will greenlight and fund the project and mobilize resources to turn your idea into reality. Show them how in-office surgery adds value to their brand and improves market differentiation and penetration. Ask how often someone would rather go to the OR if the procedure can be done in the office. Financial considerations should be made before the first incision, not after the fact.
Finally, identify your potential saboteurs. Is the OR schedule overloaded and in need of relief, or is it light, making any diversion of cases a threat? How much would anesthesia services be affected, and are they motivated to steer the organization away from in-office surgery?
Start small, prove safety, and expand deliberately
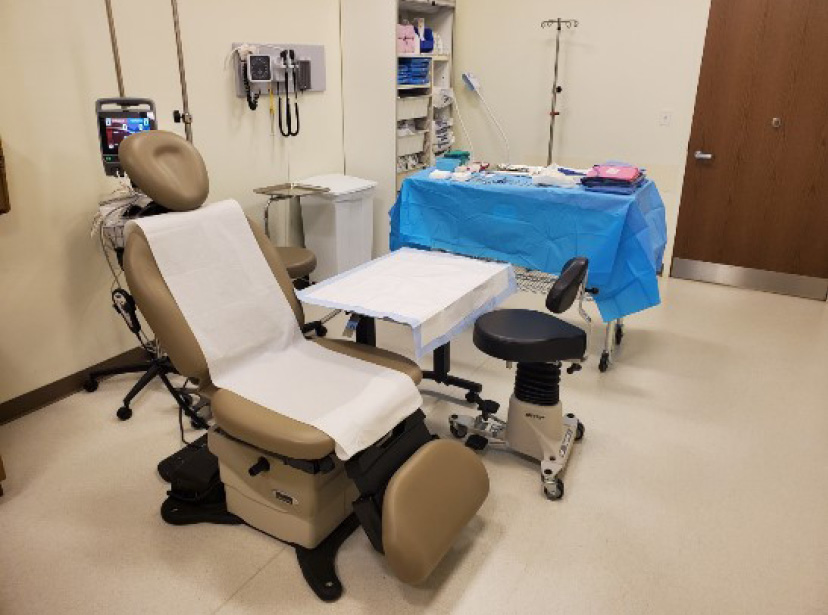
A mature in-office surgery program can handle a wide spectrum of cases, but a launch program should be modest until staff members are well versed and processes are well established. The safest starting point is a selection of simple cases that require minimal instruments and resources. A standardized room setup and predictable workflow help ensure safety and efficiency during early program implementation (Figure 2).
Consider starting with quick soft tissue procedures before introducing power instruments and imaging. Start with cases you have already mastered and that are straightforward, high volume, and low risk. Remember that everyone is watching you start, so do not go too far too fast. Stay in control. One new variable at a time is the right philosophy: Try a new setting with familiar procedures or new procedures in a familiar setting — never both simultaneously.
Train a competent team and give them ownership
In-office surgery lives or dies on the performance of the core people standing around an awake patient. Proper awake‑surgery etiquette and strict sterile techniques are essential — and so is knowing what not to do. Inappropriate jokes or casual expressions, conversations about other patients, visible disagreement among staff, or expressions of surprise — there is no room for “oops” in awake surgery — can undermine patient confidence immediately. Because staff without prior surgical training may not recognize these risks, surgeons must avoid taking behind‑the‑scenes knowledge for granted and maintain close oversight before, during, and after surgery until the team is fully competent.
Hospital-affiliated practice vs. independent practice
Quality, regulation, and reimbursement are core design constraints, no matter where in-office surgery is offered. In hospital-affiliated practices, stakeholders will keep matters aligned as they are bound by CMS and other regulations. In independent practices, regulations are less stringent and vary by state but there is no excuse for subpar patient care that does not meet licensure requirements, infection control expectations, emergency preparedness, and documentation protocols. In both settings, financial viability is critical for longevity.
The end goal for both is success that relies on having the appropriate infrastructure to provide safe, effective, and efficient surgical care and on knowing which cases belong in the office surgical suite and which should remain in the operating room. An in-office surgery program should not be a monument to a surgeon’s ego, but a disciplined extension of exemplary care that is equivalent to that provided in the operating room without the unnecessary burden and waste.
Editor’s note: This material was explored in more detail during AAOS 2026 Annual Meeting Instructional Course Lecture 352 on Wide-Awake Hand Surgery: How to Implement and Advance a Wide-Awake Practice in the Main Operating Room, Surgicenter, and Even Your Office and Symposium E Advanced Office Orthopaedics: Ultrasound, Injectables, and Surgery. Both courses are available as part of AAOS 2026 OnDemand.
Shafic Sraj, MD, MBA, FAAOS, is the director of orthopaedic surgery at the Valley Health Center for Orthopedic Excellence in Winchester, Virginia. He specializes in hand and upper extremity surgery and wide awake and in-office surgery and is an adjunct professor of orthopaedics at West Virginia University.