Patient-reported outcome measures (PROMs) are standardized methods for capturing the patient perspective. If they haven’t already entered clinical practice, they should soon.
“Historically, we have looked at success as measured by physicians, the healthcare system, and the insurer — like fracture healing, range of motion, presence of infection — but patient-reported outcomes (PROs) allow us to focus on what matters to patients from their perspective,” explained Lauren Michelle Shapiro, MD, MS, FAAOS, associate professor in residence, department of orthopaedic surgery at the University of California, San Francisco.
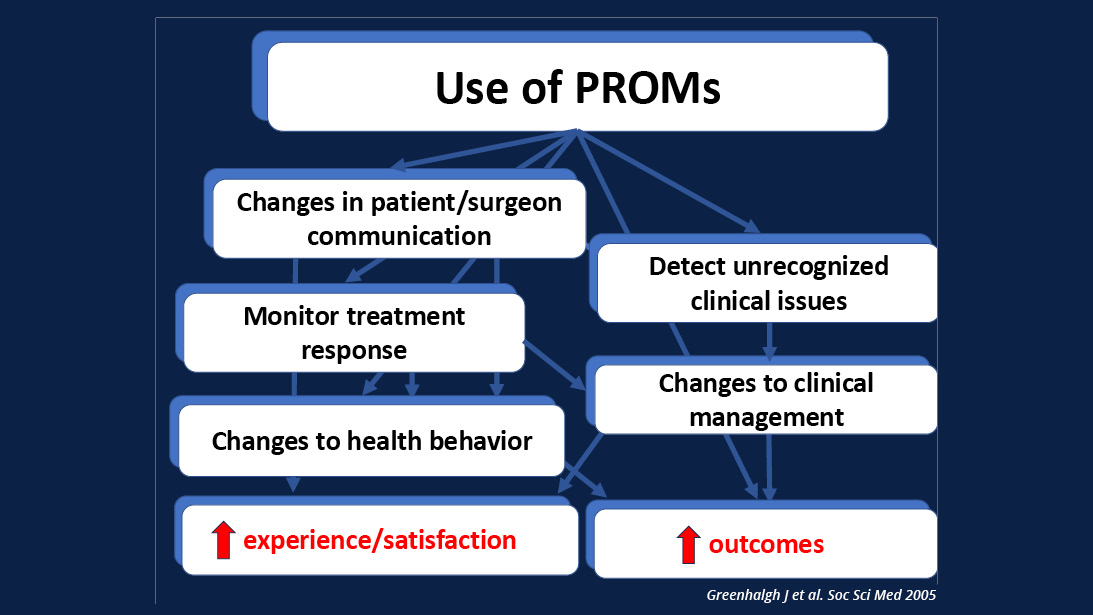
Although PROMs have more commonly been used in the research setting, their use in clinical practice and policy are increasing (Figure 1).
At the AAOS 2026 Annual Meeting, Dr. Shapiro led an Instructional Course Lecture, “PROMS Are Here to Stay: Utilizing PROMs to Benefit Patients and Minimize Financial Risk,” where, together with colleagues, she discussed why PROMs are important and how they are beginning to be more widely incorporated into orthopaedics.
Why PROMs?
In Dr. Shapiro’s view, it is time to start thinking about PROs like any other piece of data collected by physicians.
“We wouldn’t order an X-ray and then not look at it or integrate it into patient discussions and decisions,” she said. “We shouldn’t do that with PROMs, either.”
There are several ways to use PROMs to improve patient outcomes and the patient experience. For example, a 2019 study by Bernstein et al evaluated use of the Patient-Reported Outcomes Measurement Information System (PROMIS) during an orthopaedic clinic visit compared with visits without its use. The study showed that use of PROMIS had a positive impact on the patient experience; patients reported being more likely to feel the provider spent enough time with them and were more likely to recommend the provider.
PROMs can also be used to monitor peri- and postoperative treatment responses. An important study from the cancer literature evaluated the use of PROs for symptom management, including monitoring PROs and generating a report of symptom burden history for the oncologist at the patient visit. Incorporating PROs was linked with increased survival, with patients surviving an average of five months longer.
PROs can also be used to detect previously unrecognized clinical issues, changes to health behavior, and changes to clinical management. Recognition of all of these can improve patient satisfaction and outcomes.
Alphabet soup
Learning about and applying concepts such as PROs, PROMs, and PROMIS can seem like an alphabet soup at times, acknowledged Amy M. Cizik, PhD, MPH, research assistant professor in the department of orthopaedics and director of patient-reported outcomes at the University of Utah Health.
Medicine today is not just about incidence, prevalence, and survival; the field is moving beyond that. People are living, but one must also ask, “How are they living? What is their health state?” However, how that is defined has changed over the years, Dr. Cizik said. First, it was functional status and activities of daily life; later, social activities were included, then measurement of quality of life (QOL) and health-related QOL were added. Now, it is PROs.
Physicians looking to incorporate PROMs into their practice may be overwhelmed by the variety of tools and options available. Most of these tools can be divided into acute (urologic function, pain, etc.) or chronic (e.g., pain, depression, sleep, and anxiety) domains. Clinicians must ask themselves, “What are the primary things that surgery is looking to improve?” They should start to think about not only the measure but the domain of health they want to measure.
When looking into incorporating PROMs, it is also important that practices think realistically about their IT infrastructure and how these measures will not only be implemented but also how the returning data can be used.
Put data to use
Kurt Spindler, MD, FAAOS, associate chief, clinical research, professor of orthopaedics at the Cleveland Clinic, detailed some of the organization’s efforts to do just that.
Medicine, he said, suffers from a fundamental flaw. “The majority of our patients do not return to our office a year later to tell us how well or poorly they are doing,” Dr. Spindler said.
To correct that, improve follow-up, and begin the incorporation of PROs, Dr. Spindler and colleagues at the Cleveland Clinic developed the Orthopaedic Outcome Measurement and Evaluation program. The program was designed to be cost-effective, scientifically valid, and scalable and integrate effectively into the existing workflow.
In the 10 years since the program’s creation, there have been almost 150,000 surgeries eligible for inclusion, with an enrollment success rate of more than 90% for PROM collection and details on surgeon treatment. One-year follow-up was achieved in almost 75% of patients. The data also allow for information on surgeon and hospital system statistics around volume, procedure cost, and outcomes trends.
Despite this success, Dr. Spindler said the work is not yet over.
“We have captured the main design features we wanted, but we haven’t implemented this in real time in the clinic,” Dr. Spindler said. He wants to be able to take all the data gathered and use it to help make decisions about patient care. The data can help physicians predict expected outcomes, improvements, complications, and costs.
“You [need] have good data to make good decisions. If we are trying to make a decision to give a treatment that costs $30,000 or $100,000, we should have the data behind who responds and who doesn’t respond,” Dr. Spindler said. “This is the future, and PROMs are a part of it.”
PROs linked to reimbursement
The final speaker, Robin Neil Kamal, MD, FAAOS, associate professor, department of orthopaedic surgery, Stanford University, discussed the importance of PROMs from a business standpoint.
“I would venture to guess that in 10 years we are all going to be submitting PROMs in one way or another [as] part of a requirement for payments,” Dr. Kamal said.
Some of this is already evident by the growing inclusion of PROMs in accountable care models, the Centers for Medicare & Medicaid Services’ Transforming Episode Accountability Model, and the recently created ambulatory specialty models.
“From a measurement perspective, we are starting to see PROMs included in quality measure steps for these models,” Dr. Kamal said, adding that these are only likely to increase in the coming years.
“Although PROMS require additional work, changes to clinical care pathways, and financial investment, the data measured can be used to benefit patients, practices, and hospital systems,” Dr. Shapiro said.
Leah Lawrence is a freelance medical writer for AAOS Now.
References
- Bernstein DN, Fear K, Mesfin A, et al. Patient-reported outcomes use during orthopaedic surgery clinic visits improves the patient experience. Musculoskeletal Care. 2019 Mar;17(1):120-125. doi:10.1002/msc.1379. Epub 2019 Jan 7.
- Basch E, Deal AM, Dueck AC, et al. Overall survival results of a trial assessing patient-reported outcomes for symptom monitoring during routine cancer treatment. JAMA. 2017;318;(2):197-198.
- Cleveland Clinic. Research News. Studying the past of orthopaedic patient-reported outcome measures to improve the future of care. Published January 16, 2026. Accessed March 12, 2026.