Over many years, surgeons have continued to improve techniques in the repair and fixation of damaged structures. In the operating room, suture and anchor fixation and biological enhancements aid success. Multimodal pain management has also decreased the use of medications that could potentially slow or damage the healing process, as well as addressing the negative impacts of smoking and metabolic syndrome.
Despite advances in surgical technique and perioperative care, basic nutritional supplementation that could enhance the body's natural healing response remains surprisingly underexplored. Not infrequently, in attempts to optimize performance, patients rely on unproven internet or other sources of information on supplementation and then may obtain supplements of questionable purity that may cause more harm than good.
Surgeons treating athletes have an opportunity to provide evidence-based recommendations. The Tulane Department of Orthopaedic Surgery, in New Orleans, has maintained a strong interest in perioperative nutrition for the past 20 years and has frequently collaborated with Mackie Shilstone, a sports performance manager and career extension specialist who has worked with more than 3,000 professional athletes and teams over the past 43 years. Shilstone, who is also affiliated with the Tulane Department of Kinesiology, has pioneered many nutritional strategies for athletes across all age groups and skill levels, and his expertise forms the foundation of the supplement protocol currently in use at the Tulane Department of Orthopaedic Surgery. The author agrees with Shilstone that nutritional augmentation and supplementation are integral to recovery at any age. Both believe surgery of any kind is a traumatic experience, both physically and mentally, and anything we can do to improve our body's response is beneficial.
“The surgical procedures required to repair rotator cuff trauma exacerbate soft tissue damage,” Shilstone said, “therefore increasing recovery time, especially for patients older than 40 years of age, who are contending with anabolic resistance, sarcopenia, and dynapenia.
“Much like anaerobic-type exercise, such as isotonic resistance training, where you tear down and rebuild tissue to accelerate skeletal muscle growth, performance nutrition supplementation is a mainstay to the repair and recovery process before, during, and post-training. I believe the same can be said to achieve a successful surgical outcome,” he added.
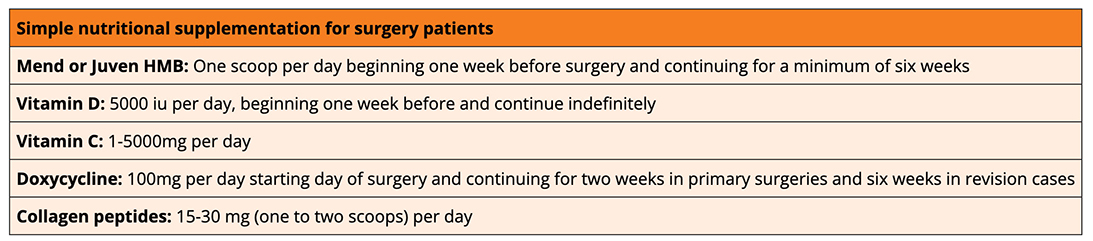
The department selected supplements based on the available scientific evidence and then evaluated their impact by studying healing outcomes in rotator cuff patients, using postoperative ultrasound to assess differences. The department noted an increase of 1 to 2 mm in the measured thickness of the supraspinatus tendon at six and 12 weeks postoperatively in those patients taking the supplements as compared to those who did not. This article focuses on that specific experience rather than serving as a comprehensive review of perioperative nutritional support.
High-quality protein fuels the body's repair process
Protein is one of the fundamental building blocks of healing, especially when it is of high quality and rich in essential amino acids. Our Tulane Institute of Sports Medicine team of physicians primarily use two protein-based supplementation products, Juven HMB and Mend, both of which offer strong nutritional profiles and demonstrate the ability to increase collagen production at the wound site.
Critical components of effective protein support include:
- HMB (beta-hydroxy-beta-methylbutyrate), which helps protect muscle cells from breakdown and supports muscle mass preservation;
- arginine, which enhances blood flow and drives protein production; and
- additional elements — such as glutamine, collagen peptides, and micronutrients — that contribute to tissue repair.
Creatine monohydrate may be included in these protein supplements or added separately, as it also helps build muscle. Most supplements use some version of high-quality whey protein, but there are options without milk and associated byproducts for those who are lactose intolerant.
In older patients, the team closely monitors albumin levels, along with calcium and vitamin D, to add nutritional support for both healing and recovery.
Higher perioperative vitamin D levels can strengthen the healing response
Vitamin D plays a crucial role in tendon healing. Population studies indicate that up to 70% of individuals tested demonstrate vitamin D deficiency. Beyond its well-known partnership with calcium in maintaining healthy bone structure, vitamin D supports tendon healing and turnover in day-to-day activities. It influences both tendon-to-bone healing and the quality of the tendon itself. It also helps inhibit mineral metalloproteinase formation. Many clinicians now advocate for higher perioperative vitamin D levels — often in the 70-80 ng/ml range — rather than the traditionally accepted threshold of anything above 30 ng/ml.
Collagen peptides and vitamin C support tendon repair
Vitamin C and collagen peptides contribute to tendon healing by supporting collagen formation and strengthening tissue repair. Collagen peptides are an excellent source of amino acid building blocks, such as glycine and proline, that have been shown to stimulate collagen formation. Combining collagen peptide supplementation of 10-15 grams with 1000-5000 mg of vitamin C will provide best results in adding quality collagen to the repair site.
Doxycycline helps protect healing tissue
Catabolic factors that may inhibit tendon and bone healing include the matrix metalloproteinases (MMPs). This family of enzymes break down extracellular matrixes, particularly collagen, and are commonly found in the lateral bursal tissue of the shoulder. According to research from Del Buono and colleagues, the antibiotic doxycycline has been quite useful as an antagonist to MMP activity and can help reduce the catabolic effects. Doses as low as 20 mg per day may be effective in decreasing the effects of MMPs on healing, but intake of 100 mg once or twice a day may also work, with the added advantage of being effective in managing C acnes infection or contamination.
Interest in emerging peptides is growing
More recent substances that may be beneficial but remain insufficiently studied include gastric peptides such as BPC-157, TB-500, and human growth hormone. Researchers have explored gastric peptides for their potential positive effects on healing muscle tendon, ligaments, and bones by boosting growth factors. Although BPC-157 was initially banned by the World Anti-Doping Agency (WADA), it was later removed from the prohibited list after research showed no measurable impact on athletic performance; however, it is not approved for human use. TB-500, a synthetic peptide, has shown some effects on strength in an equine model, but human data are lacking. Despite the absence of clinical evidence, some individuals currently use BPC-157 and TB-500 in combination, believing they may enhance healing outcomes. Rigorous scientific study is still needed to determine whether these substances offer verifiable benefits and to guide appropriate patient counseling.
One of the limitations in advising patients as orthopaedic surgeons is the lack of evidence on these potentially beneficial substances. Patients may use them on their own, relying on word of mouth or even non-surgeon physician recommendation without understanding the complexity of the healing process from surgery. Surgeons need to be open to considering which of these supplements can be used to benefit patients, while also recognizing the responsibility to guide patients toward safe, evidence-based care.
Felix H. “Buddy” Savoie III, MD, FAAOS, is the Ray Haddad Professor and chair of the department of orthopaedic surgery at Tulane University, New Orleans. He is a past president of AAOS, the American Shoulder and Elbow Surgeons, the Arthroscopy Association of North America, and the Louisiana Orthopaedic Association. He is also the honorary past president of the Global Elbow Network.
References
- Yeo, MHX., Seah, SJS; Tay, HW; Lie, D. Preoperative serum vitamin D deficiency is associated with increased rotator cuff fatty degeneration but is unlikely to influence post repair outcomes: a systematic review and meta-analysis of correlation coefficients. JSES Rev Rep Tech. 2025;5(3) 444-452. doi.org/10.1016/j.xrrt.2025.02.006
- Bouchard, MD, Dagher, D, Keogh, C, Alqahtani, KM. The role of vitamin D in postoperative tendon healing: a scoping review. Orthop J Sports Med. 2025;13(10):23259671251371300. doi:10.1177/23259671251371300
- Williams, D, Wischmeyer, PE,. Perioperative nutrition care of the orthopedic srgery patient. Tech Orthop 2019;35(1):15-18. doi:10.1097/BTO.00000000000000412.
- Khatri, M, Naughton, R, Clifford, T, Harper, L, Corr, L. The effects of collagen peptide supplementation on body composition, collagen synthesis and recovery from joint injury and exercise, a systematic review. Amino Acids. 2021;53(10): 1493-1506 doi:10.1007/s00726-021-03072-x
- Del Buono, A, Loiva, F, Longo, U, et al. Metalloproteases and rotator cuff disease. J Shoulder Elbow Surg. 2021;21(2): 200-208. doi.org/10.1016/j.jse.2011.10.020
- Vasireddi, N, Hahamyan, H, Salata, M, et al. Emerging use of BPC-157 in orthopaedic sports medicine: a systematic review. HSS J. 2025. doi:10.1177/15563316251355551