The AAOS Clinical Practice Guideline (CPG) for the Prevention of Total Hip and Knee Arthroplasty Periprosthetic Joint Infection (PJI), released in November 2024, has become one of the most widely viewed CPGs, used by orthopaedic and dental professionals alike. Following the subsequent release of the updated Appropriate Use Criteria (AUC) for the Management of Patients with Orthopaedic Implants Undergoing Dental Procedures, the Association for Dental Safety (ADS) invited AAOS to further explore the topic with its members.
More than 600 ADS members attended the webinar, “Antibiotic Prophylaxis: Weighing the Risks and Benefits, Has the Scale Changed?” The ADS, formerly known as the Organization for Safety, Asepsis and Prevention, is the only dental membership association for oral healthcare professionals, focused exclusively on dental infection prevention and patient and provider safety. The webinar featured orthopaedic surgeon Matthew J. Grosso, MD, FAAOS, and dentist Erinne Kennedy, DMD, MPH, MMSc, who presented the clinical evidence on antibiotic use and perspectives on interprofessional collaboration.
The webinar reviewed the current evidence of the CPG and the AUC on antibiotic prophylaxis, discussed gaps in the existing literature, and examined how clinicians can apply this evidence to inform decision making when prescribing antibiotics. Attendees received continuing education credit for their participation. AAOS members may access this educational webinar, developed to promote patient safety, as a part of their professional development.
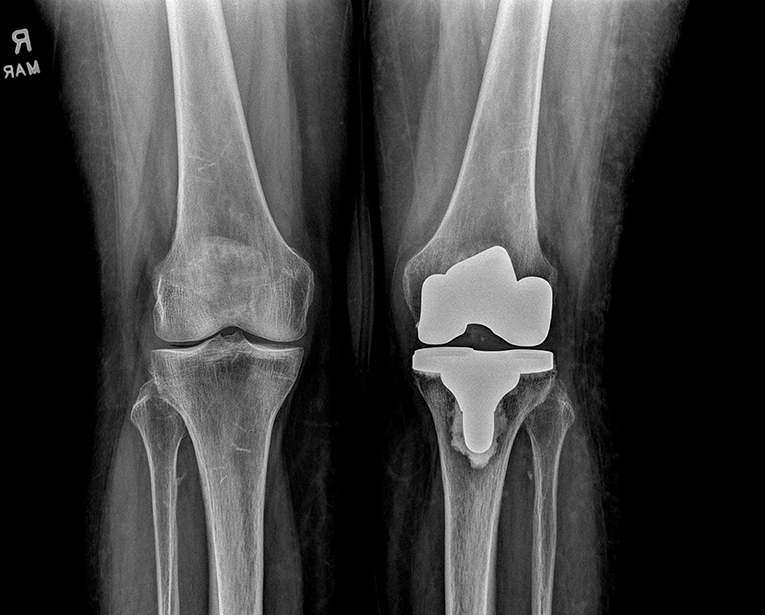
“Hip and knee replacements are among the most common orthopaedic procedures, and PJI affects 1-2% of primary hip and knee replacement procedures from hematogenous spread, contiguous spread from a local source, or surgical site infection from the index procedure,” Dr. Grosso said. “These patients also routinely receive dental care, and orthopaedic surgeons and dentists are frequently asked whether and when a patient should receive antibiotics prior to a dental procedure.”
Dr. Kennedy emphasized that effective antibiotic stewardship for patients with total joint replacements requires interprofessional communication.
“Decision making for these patients often involves dental teams and orthopaedic surgeons,” Dr. Kennedy explained. “ADS and AAOS wanted to create a space where these perspectives are shared because understanding each other's approach is essential to supporting safe, coordinated care. By creating a space where all healthcare teams can learn together and ask questions, we build an environment that allows for better decision making chairside.”
A key takeaway from this discussion was that routine use of a systemic prophylactic antibiotic prior to a dental procedure in patients with a hip or knee replacement may not reduce the risk of
a subsequent periprosthetic joint infection. Under the current CPG and AUC, prophylactic antibiotics are considered possibly appropriate only for immunocompromised patients undergoing an invasive dental procedure.
Additional highlights from the webinar included:
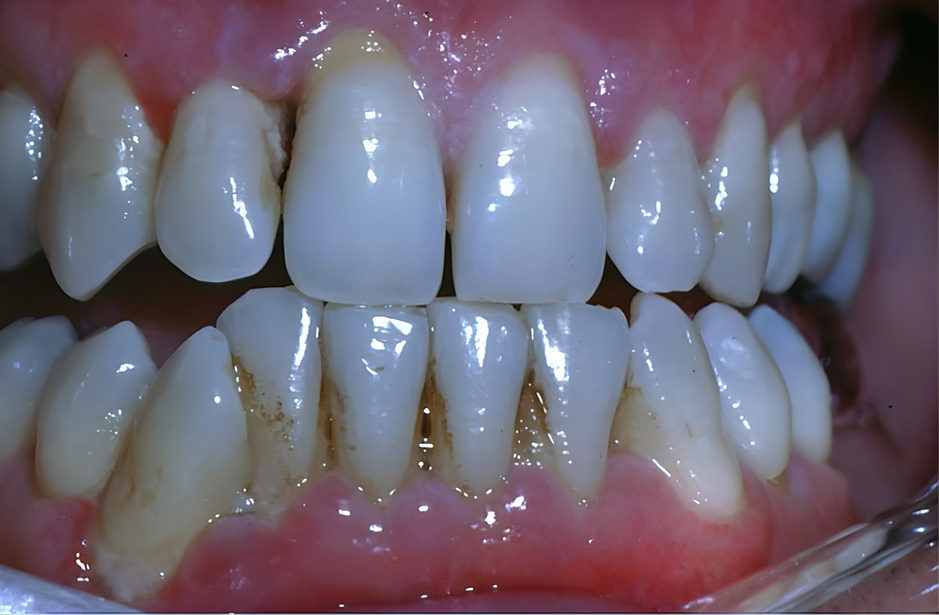
- Dental procedures pose no greater risk for systemic bacteremia than activities of daily living, such as brushing teeth or eating.
- The use of antibiotic prophylaxis may pose unnecessary risk of adverse drug reactions and/or antibiotic resistance.
- Recommendations for antibiotic prophylaxis should be individualized for each patient based on their medical history.
“Given the large number of registrants for this webinar, ADS members are interested in this emerging topic,” said Michelle Lee, executive director of ADS. “The organization has been focused on infection prevention and control (IP&C). Antibiotic stewardship, a global and very important patient safety issue, fits well with IP&C. In fact, ADS has developed a standard operating procedure that embeds antibiotic stewardship into IP&C's daily activities, increasing the likelihood of its successful practice. ADS members will help bring the new AAOS CPG and AUC to dentistry. Our joint webinar was an excellent start toward this goal.” The full CPG and AUC are available through AAOS' OrthoGuidelines website and free mobile app.
Jennifer Lefkowitz is a freelance writer for AAOS Now.
Appropriate Use Criteria for antibiotic prophylaxis before dental procedures
The scope of this AUC is to assess clinical situations in which antibiotic prophylaxis prior to dental procedures in “average” or “lower” risk patients is indicated to reduce the theoretical risk of post-surgical prosthetic joint infection.
Currently, there are no data to guide clinical decisions for a small subset of higher-risk patients, such as those with revision implants, megaprostheses, poor soft tissue envelopes, or prior prosthetic joint infection.
When an orthopaedic surgeon discusses the role of antibiotic prophylaxis with a patient before a dental procedure, it is also important to encourage routine, proper dental care and hygiene as an equally important infection-prevention measure. Appropriate dental care is always recommended.
To support clinical decision making, the AUC online tool provides guidance based on two patient indicators: the level of invasiveness of the dental procedure and the systemic host status (immunocompetent or immunocompromised).
Definitions:
1. Level of Invasiveness
Noninvasive procedures include:
- dental examination without probing dental radiograph or cone beam CT imaging, denture adjustment procedures, clear orthodontic aligner (invisible braces) adjustment procedures, occlusal guard or bite splint adjustment;
- oral hygiene procedures including dental cleaning, dental prophylaxis using a rubber cup and handpiece (without scaling), or periodontal probing (without SRP);
- orthodontic procedures including banding or debanding orthodontic fixes or removable appliances, archwire adjustment, orthodontic mini-implant removal, and orthodontic separate placement; and
- other noninvasive procedures including suture removal, anesthetic injection, crown and bridge placement, dental restorative procedures, rubber dam clamp or matrix band wedge between teeth, impression taking, and endodontic treatment (root canal therapy).
Invasive procedures include:
- scaling and/or root planing (SRP) with manual (hand instruments) or ultrasonic scaler;
- dental extractions, including single, multiple, and impacted third molar;
- oral surgery (including dental implant surgery, periodontal surgery, cleft palate surgery, piezoelectric surgery, osteosynthesis plate removal); and
- treatment of active dental infection.
2. Systemic host status
Immunocompromised
- For a comprehensive list of conditions that are defined by the Centers for Disease Control and Prevention guidelines as severely immunocompromised, please see the following citation linked here.